Calprotectin Stool Test Instructions: A Comprehensive Guide
Calprotectin testing aids in distinguishing inflammatory bowel conditions‚ potentially reducing the need for invasive procedures. It’s a sensitive assay measuring intestinal inflammation‚ increasingly utilized for screening and monitoring.
What is the Calprotectin Stool Test?
The calprotectin stool test is a non-invasive laboratory assessment utilized to detect inflammation within the gastrointestinal tract. It measures the concentration of calprotectin‚ a protein released by neutrophils – a type of white blood cell – when inflammation is present. This test is performed on a sample of your stool (feces) and provides valuable insights into the health of your digestive system.
Unlike tests searching for blood‚ calprotectin specifically identifies inflammation‚ making it a highly sensitive indicator of intestinal issues. Gastroenterologists are increasingly relying on this test to both screen for and monitor various gastrointestinal conditions‚ offering a crucial step in diagnosis and treatment planning. It’s a key tool in modern digestive health assessment.

Why is the Calprotectin Stool Test Performed?
The calprotectin stool test is primarily performed to help determine if intestinal symptoms are caused by inflammatory conditions or non-inflammatory ones‚ like Irritable Bowel Syndrome (IBS). It assists in differentiating between these‚ as IBS doesn’t show elevated calprotectin levels.
This test can potentially eliminate the need for more invasive procedures‚ such as colonoscopies‚ if calprotectin levels are low. Doctors use it to investigate persistent diarrhea‚ abdominal pain‚ or changes in bowel habits. Furthermore‚ it’s valuable for monitoring individuals already diagnosed with inflammatory bowel disease (IBD)‚ assessing disease activity and response to treatment.
Conditions Detected by Calprotectin
Calprotectin is a highly sensitive marker for inflammation within the intestinal tract‚ making it crucial in detecting various gastrointestinal conditions. Primarily‚ it’s used to identify and assess Inflammatory Bowel Disease (IBD)‚ encompassing both Crohn’s Disease and Ulcerative Colitis. Elevated levels strongly suggest the presence of intestinal inflammation characteristic of these conditions.

Importantly‚ the test excels at distinguishing IBD from Irritable Bowel Syndrome (IBS)‚ where calprotectin levels typically remain normal. While not a direct diagnostic tool for cancer‚ it can indicate inflammation needing further investigation‚ potentially uncovering underlying issues.
Inflammatory Bowel Disease (IBD) – Crohn’s Disease
In Crohn’s Disease‚ calprotectin levels are typically elevated‚ reflecting the chronic inflammation affecting various parts of the digestive tract. This test assists in diagnosing Crohn’s‚ differentiating it from other conditions with similar symptoms. Monitoring calprotectin levels helps assess disease activity and response to treatment‚ guiding therapeutic decisions.
High calprotectin indicates ongoing inflammation‚ potentially prompting adjustments to medication or further investigations like endoscopy. Conversely‚ decreasing levels suggest treatment effectiveness. However‚ calprotectin doesn’t pinpoint the exact location or extent of Crohn’s inflammation; further imaging is often required.
Inflammatory Bowel Disease (IBD) – Ulcerative Colitis

Ulcerative colitis‚ characterized by inflammation limited to the colon‚ also demonstrates elevated calprotectin levels in stool samples. The test’s sensitivity makes it valuable for initial diagnosis‚ particularly when distinguishing IBD from functional bowel disorders. Regular calprotectin monitoring aids in assessing disease remission and detecting flares‚ allowing for proactive management.
Increased calprotectin levels correlate with the extent and severity of colonic inflammation‚ providing insights into disease activity. While helpful‚ calprotectin doesn’t replace colonoscopy‚ which remains crucial for visualizing the intestinal lining and obtaining biopsies. It’s a powerful tool alongside traditional diagnostic methods.

Distinguishing IBD from Irritable Bowel Syndrome (IBS)
A key application of the calprotectin stool test is differentiating Inflammatory Bowel Disease (IBD) from Irritable Bowel Syndrome (IBS). IBS is a functional gastrointestinal disorder without detectable inflammation‚ resulting in typically low calprotectin levels. Conversely‚ IBD – Crohn’s disease and ulcerative colitis – consistently exhibits high calprotectin concentrations.
This distinction is crucial‚ as treatment strategies differ significantly. Elevated calprotectin suggests the need for further investigation‚ like colonoscopy‚ to confirm IBD. Low levels can support an IBS diagnosis‚ potentially avoiding unnecessary invasive procedures. It’s a valuable first-line test in patients presenting with chronic bowel symptoms;
Preparing for the Calprotectin Stool Test
Proper preparation is vital for accurate calprotectin stool test results. While generally requiring minimal preparation compared to colonoscopies‚ certain considerations are important. Discuss all medications with your doctor‚ as some – particularly NSAIDs – can cause intestinal inflammation and falsely elevate calprotectin levels.
Dietary adjustments are usually not strictly necessary‚ however‚ informing your physician about any existing gastrointestinal conditions or recent infections is crucial. These factors can influence test outcomes. Follow your doctor’s specific instructions carefully‚ as protocols may vary slightly between healthcare providers and laboratories.
Dietary Considerations Before the Test
Generally‚ no specific dietary restrictions are mandated before a calprotectin stool test. Unlike some other stool tests‚ you typically don’t need to follow a special diet. However‚ maintaining your usual eating habits is recommended. Avoid significant changes to your diet in the days leading up to sample collection‚ as this could potentially influence the results.
There’s no need for a low-fiber or clear liquid diet. Continue consuming a normal‚ balanced diet. If you have specific dietary concerns or questions‚ consult your healthcare provider for personalized guidance. Consistency in your diet is key to obtaining the most reliable test outcome.
Medication Interference
Certain medications can potentially interfere with calprotectin stool test results‚ though the impact is generally considered minimal. Nonsteroidal anti-inflammatory drugs (NSAIDs)‚ such as ibuprofen and naproxen‚ may cause intestinal inflammation‚ potentially elevating calprotectin levels. However‚ discontinuing these medications solely for the test isn’t usually advised – continue taking them as prescribed.

Inform your doctor about all medications you are taking‚ including over-the-counter drugs‚ supplements‚ and herbal remedies. They will assess whether any adjustments are necessary. Corticosteroids can also influence results‚ so transparency is crucial for accurate interpretation.
Informing Your Doctor About Existing Conditions
It’s vital to disclose all existing medical conditions to your doctor before undergoing a calprotectin stool test. Specifically‚ a history of inflammatory bowel disease (IBD)‚ such as Crohn’s disease or ulcerative colitis‚ is crucial information. Previous gastrointestinal surgeries or significant digestive issues should also be reported.
Conditions affecting the immune system‚ or those requiring immunosuppressant medications‚ may influence test results. Your doctor needs a complete medical picture to accurately interpret the calprotectin levels and determine the appropriate next steps. Open communication ensures the test’s effectiveness in guiding your care.
Collecting the Stool Sample: Step-by-Step Instructions
Careful sample collection is paramount for accurate calprotectin testing. Your kit will contain specific containers and instructions – follow them precisely. Typically‚ you’ll collect a small stool sample directly into the provided container‚ avoiding contact with toilet water. Use the provided scoop or applicator to obtain the sample.

Ensure the container is securely sealed after collection. Proper technique minimizes contamination‚ which can skew results. Most kits require multiple samples collected over several days for a comprehensive assessment. Adhering to these steps guarantees reliable data for your healthcare provider’s analysis.
Materials Provided in the Collection Kit
Your calprotectin stool test kit will contain everything needed for successful sample collection. Expect to find one or more collection containers‚ specifically designed to preserve the sample integrity. A plastic scoop or applicator is included for easy and hygienic stool retrieval‚ minimizing contact.
Detailed‚ step-by-step instructions are crucial; read them thoroughly before beginning. Some kits may also include gloves‚ a biohazard bag for safe disposal‚ and a pre-paid shipping label for convenient laboratory submission. Verify all components are present before proceeding to ensure a complete and accurate testing process.
Proper Collection Technique
Accurate collection is vital for reliable results. After using the toilet‚ collect a small amount of stool – about the size of a walnut – using the provided scoop. Avoid flushing the toilet before collecting‚ as this can contaminate the sample. Ensure the stool is not mixed with urine or water.
Carefully transfer the sample into the collection container‚ following the kit’s specific instructions. Securely close the container‚ avoiding spillage. Wash your hands thoroughly with soap and water after handling the sample and any collection materials. Proper technique minimizes errors and ensures accurate assessment of intestinal inflammation.
Avoiding Contamination of the Sample
Maintaining sample purity is crucial for accurate calprotectin levels. Avoid collecting stool that contains visible traces of blood‚ as this can falsely elevate results. Do not allow urine to mix with the stool sample during collection; this significantly impacts accuracy.
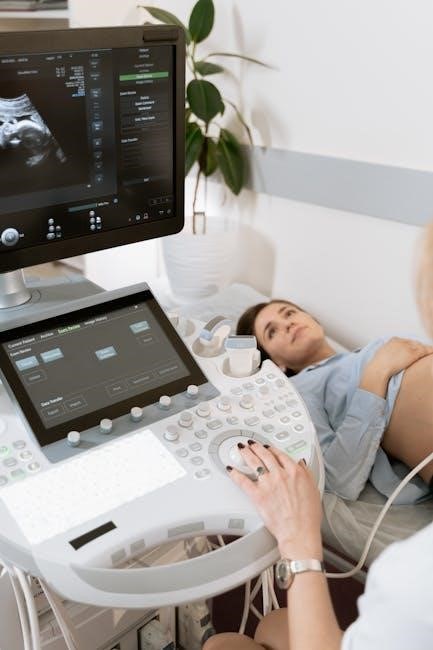
Ensure the collection container is clean and dry before use‚ and avoid touching the inside of the container or the collection scoop. Thorough handwashing before and after the process is essential. Contamination can lead to misdiagnosis‚ so meticulous attention to detail during collection is paramount for reliable testing.
Sample Storage and Handling
Proper storage and handling are vital for preserving sample integrity. Following collection‚ immediately store the sample as instructed by your kit – typically refrigeration is required. Most labs prefer samples to be refrigerated‚ maintaining a temperature between 2-8°C (35-46°F).
Adhere strictly to the specified time limit for submission; delays can degrade the sample and affect results. Typically‚ samples should reach the lab within 72 hours of collection. Ensure the packaging is secure to prevent leakage or damage during transport‚ following the kit’s guidelines precisely.
Temperature Requirements for Storage
Maintaining the correct temperature is crucial for accurate calprotectin measurements. Most laboratories require stool samples to be refrigerated promptly after collection‚ ideally within a few hours. The optimal storage temperature generally falls between 2-8°C (35-46°F).
Freezing is typically not recommended unless specifically instructed by the laboratory‚ as freeze-thaw cycles can compromise the sample’s integrity. Always verify the specific temperature guidelines provided with your collection kit‚ as variations may exist between different testing facilities. Proper temperature control minimizes degradation and ensures reliable test results.
Time Limit for Sample Submission
Prompt submission of the stool sample is essential for reliable calprotectin testing. Degradation of calprotectin can occur over time‚ even with proper refrigeration‚ potentially affecting the accuracy of results. Most laboratories specify a maximum timeframe for sample acceptance‚ typically within 72 hours of collection.

However‚ this timeframe can vary‚ so it’s vital to confirm the specific requirements with your healthcare provider or the designated testing facility. Samples submitted beyond the recommended timeframe may be rejected or yield inaccurate readings. Adhering to the submission deadline ensures the most dependable assessment of intestinal inflammation.
Packaging the Sample for Transport
Proper packaging is crucial to maintain sample integrity during transport to the laboratory. The collection kit typically includes a sealed‚ leak-proof container and a biohazard bag. Ensure the sample container is securely closed to prevent spillage or contamination. Place the container inside the biohazard bag and seal it tightly.
Follow any specific packaging instructions provided with your kit. Some labs may require additional packaging‚ like absorbent material‚ to contain potential leaks. Clearly label the package with the necessary patient information and any required laboratory details. Transport the sample promptly‚ adhering to the specified temperature requirements.
Understanding the Test Results
Calprotectin levels are interpreted in conjunction with your medical history and other test results. High calprotectin levels generally indicate inflammation within the intestinal tract‚ suggesting a condition like Inflammatory Bowel Disease (IBD). Conversely‚ low levels suggest inflammation is unlikely‚ potentially pointing towards non-inflammatory conditions like Irritable Bowel Syndrome (IBS).
However‚ results aren’t definitive. False positives and negatives can occur. A high result doesn’t automatically confirm IBD‚ and further investigation is usually needed. A low result doesn’t entirely rule it out. Your doctor will discuss the results and determine the next steps‚ which may include colonoscopy or other diagnostic tests.
What Do High Calprotectin Levels Indicate?
Elevated calprotectin levels strongly suggest the presence of intestinal inflammation. This doesn’t pinpoint a specific diagnosis‚ but it indicates that something is irritating or damaging the bowel lining. Typically‚ high levels are associated with Inflammatory Bowel Disease (IBD)‚ encompassing Crohn’s Disease and Ulcerative Colitis.
However‚ other conditions can also cause elevated levels. Infections‚ certain medications‚ and even recent bowel preparation can contribute. A high result prompts further investigation‚ often involving colonoscopy with biopsies‚ to determine the underlying cause of the inflammation and establish an accurate diagnosis. It’s a crucial indicator for prioritizing further testing.
What Do Low Calprotectin Levels Indicate?
Low calprotectin levels generally suggest that significant intestinal inflammation is unlikely to be present. This is reassuring and can often rule out Inflammatory Bowel Disease (IBD) as the cause of gastrointestinal symptoms. It’s particularly helpful in differentiating IBD from Irritable Bowel Syndrome (IBS)‚ where calprotectin levels are typically normal.
However‚ a low result doesn’t entirely exclude all bowel issues. It doesn’t detect all gastrointestinal problems‚ and some conditions might not cause a substantial increase in calprotectin. Your doctor will consider the low result alongside your symptoms‚ medical history‚ and other test results to reach a comprehensive diagnosis.
False Positive and False Negative Results
While highly accurate‚ calprotectin tests aren’t foolproof; both false positive and false negative results can occur. A false positive indicates inflammation when none exists‚ potentially leading to unnecessary investigations like colonoscopies. This can happen due to minor‚ temporary inflammation or sample contamination.
Conversely‚ a false negative suggests no inflammation when it’s actually present. This might occur if inflammation is localized‚ the sample wasn’t collected correctly‚ or levels are low at the time of testing. It’s crucial to discuss any discrepancies between test results and your symptoms with your doctor for appropriate follow-up.
Calprotectin Testing and Colorectal Cancer Screening
Calprotectin is primarily an inflammation marker‚ not a direct colorectal cancer screening tool. However‚ it plays an indirect role. While it doesn’t detect cancer itself‚ elevated calprotectin levels can indicate inflammation that warrants further investigation‚ potentially leading to cancer detection.
Current colorectal cancer screening programs largely rely on the Fecal Occult Blood Test (FOBT). Calprotectin isn’t typically used as a primary screening method‚ but it can help triage patients flagged by FOBT‚ distinguishing between inflammatory conditions and potential cancer requiring colonoscopy. It aids in optimizing resource allocation within screening programs.
The Role of Calprotectin in Gastric Cancer Screening
Research explores calprotectin’s potential in gastric cancer screening‚ particularly within national cancer screening programs. Studies in Korea investigated the impact of calprotectin measurement on stage distribution of gastric cancer detected through mass screening.
Currently‚ gastric cancer screening primarily utilizes methods like endoscopy. Calprotectin isn’t a standard first-line screening tool for gastric cancer‚ but its ability to detect gastrointestinal inflammation suggests a possible role in identifying high-risk individuals who might benefit from earlier endoscopic evaluation. Further research is needed to define its precise utility and integration into existing protocols.
Calprotectin vs. Fecal Occult Blood Test (FOBT)
Calprotectin and the Fecal Occult Blood Test (FOBT) are both stool-based tests‚ but they detect different things. FOBT primarily identifies blood in the stool‚ indicating potential colorectal cancer or polyps‚ forming the basis of many colorectal cancer screening programs.
Calprotectin‚ however‚ measures inflammation in the intestinal tract. While FOBT can be positive with both inflammatory and cancerous conditions‚ calprotectin helps differentiate between inflammatory bowel disease (IBD) and other causes of gastrointestinal symptoms. Calprotectin is more sensitive for detecting intestinal inflammation than FOBT‚ guiding further investigation.
Different Calprotectin Test Technologies
Several technologies are employed for measuring fecal calprotectin‚ each with varying characteristics. Enzyme-Linked Immunosorbent Assay (ELISA) is a commonly used laboratory-based method‚ offering quantitative results. Many NHS (England) tests utilize ELISA for accurate measurement.
Calprotectin tests can be either quantitative or qualitative. Quantitative tests provide a precise numerical value for calprotectin concentration‚ aiding in disease monitoring and assessing inflammation levels. Qualitative tests simply indicate the presence or absence of elevated calprotectin‚ useful for initial screening. The choice depends on clinical needs and available resources.
ELISA (Enzyme-Linked Immunosorbent Assay)
ELISA is a widely utilized laboratory technique for quantifying fecal calprotectin levels. It involves using antibodies to detect and measure the amount of calprotectin present in the stool sample. This method is known for its sensitivity and specificity‚ providing reliable results for assessing intestinal inflammation.
Many fully quantitative laboratory-based tests available within the NHS in England rely on ELISA technology. The process involves several steps‚ including coating a plate with antibodies‚ adding the sample‚ and detecting the antibody-calprotectin complex using an enzyme-linked reaction‚ ultimately generating a measurable signal proportional to calprotectin concentration.
Quantitative vs. Qualitative Calprotectin Tests
Calprotectin tests differ in how they report results: quantitatively or qualitatively. Quantitative tests provide a precise numerical value representing the calprotectin concentration in the stool‚ typically measured in micrograms per gram of feces (µg/g). This allows for detailed monitoring of disease activity and response to treatment.
Qualitative tests‚ conversely‚ simply indicate whether calprotectin levels are above or below a predefined threshold. While less detailed‚ they are still valuable for initial screening and identifying patients who may benefit from further investigation‚ like colonoscopy. The choice between the two depends on the clinical context and the information needed.
Calprotectin Testing in the NHS (England)
The National Health Service (NHS) in England utilizes several faecal calprotectin tests for inflammatory bowel disease (IBD) diagnosis and management. Many of these tests are fully quantitative and laboratory-based‚ frequently employing Enzyme-Linked Immunosorbent Assay (ELISA) technology for accurate measurement.
The Diagnostics Advisory Committee has evaluated faecal calprotectin testing‚ recognizing its value in identifying clinically significant gastrointestinal findings. This widespread adoption reflects the test’s ability to aid in appropriate referral pathways‚ potentially reducing unnecessary colonoscopies and improving patient care within the NHS system.
Calprotectin Levels and Disease Monitoring
Gastroenterologists increasingly rely on faecal calprotectin to both screen for and monitor patients with Inflammatory Bowel Disease (IBD). Measuring calprotectin levels allows clinicians to assess disease activity‚ providing valuable insights into the extent of intestinal inflammation.
Furthermore‚ calprotectin testing can assist in predicting potential IBD relapses. Rising levels often precede clinical symptoms‚ enabling proactive adjustments to treatment plans. This proactive approach aims to maintain remission and improve long-term outcomes for individuals managing chronic inflammatory conditions of the bowel.
Monitoring Disease Activity in IBD
Faecal calprotectin serves as a crucial biomarker for objectively assessing inflammation within the intestinal tract in individuals with Inflammatory Bowel Disease (IBD). Unlike subjective symptom reporting‚ calprotectin provides a quantifiable measure of disease activity‚ aiding in treatment decisions.
Regular monitoring with calprotectin levels helps determine if current therapies are effectively controlling inflammation. Increases suggest a loss of response‚ prompting consideration of alternative or intensified treatment strategies. This allows for personalized management‚ optimizing patient care and minimizing long-term complications associated with uncontrolled IBD.
Predicting Relapses in IBD

Rising calprotectin levels‚ even within the normal range‚ can often precede clinical relapse in patients with Inflammatory Bowel Disease (IBD). This predictive capability allows for proactive intervention‚ potentially preventing severe flare-ups and hospitalizations.
Monitoring calprotectin trends enables clinicians to identify ‘silent inflammation’ – inflammation present without noticeable symptoms. Early detection of escalating levels facilitates timely adjustments to medication‚ aiming to suppress inflammation before it manifests as a full-blown relapse. This approach contributes to improved long-term disease control and quality of life for IBD patients.
The Future of Calprotectin Testing
The evolution of calprotectin testing is focused on accessibility and enhanced diagnostic capabilities. Point-of-care (POC) testing‚ offering rapid results directly in the clinic‚ is a significant advancement‚ reducing turnaround times and facilitating immediate clinical decisions.
Research is exploring the combination of calprotectin with other biomarkers to improve the accuracy of IBD diagnosis and risk stratification. These novel approaches aim to personalize treatment strategies and predict individual patient responses. Further development promises more refined monitoring and a deeper understanding of disease mechanisms‚ ultimately leading to better patient outcomes.
Point-of-Care Calprotectin Testing
Point-of-care (POC) calprotectin testing represents a significant leap forward in gastrointestinal diagnostics‚ bringing analysis directly to the patient’s location. This eliminates the delays associated with sending samples to central laboratories‚ providing results within minutes rather than days.
POC testing streamlines the diagnostic pathway‚ enabling quicker clinical decisions and potentially reducing patient anxiety. It’s particularly valuable in primary care settings where immediate assessment is crucial. The convenience and speed of POC testing are poised to expand the accessibility of calprotectin analysis‚ improving patient care and management of inflammatory bowel conditions.
New Biomarkers in Combination with Calprotectin
While calprotectin is a robust indicator of intestinal inflammation‚ research is actively exploring the benefits of combining it with other biomarkers for enhanced diagnostic accuracy. This multi-marker approach aims to refine risk stratification and personalize treatment strategies for patients with suspected inflammatory bowel disease (IBD).
Potential biomarkers include fecal microbial markers‚ specific antibody levels‚ and genetic signatures. Integrating these with calprotectin could differentiate between various IBD subtypes‚ predict disease course‚ and identify patients most likely to respond to specific therapies‚ ultimately improving patient outcomes and optimizing healthcare resource allocation.
Potential Limitations of the Calprotectin Stool Test
Although highly sensitive‚ the calprotectin stool test isn’t without limitations. Elevated levels indicate intestinal inflammation‚ but don’t pinpoint the cause – it could be IBD‚ infection‚ or even certain medications. Conversely‚ low levels don’t entirely rule out IBD‚ particularly in early stages or with limited disease extent.
False positives can occur due to NSAID use or recent intestinal infections. False negatives are possible with isolated colonic inflammation or improper sample collection. Therefore‚ results must always be interpreted in conjunction with clinical presentation‚ endoscopic findings‚ and other diagnostic tests for a comprehensive assessment.
Where to Get the Test Done
Calprotectin stool tests are primarily offered through healthcare providers and diagnostic laboratories. Your physician can order the test‚ and samples are typically collected at home using a kit they provide. Several faecal calprotectin tests are available within the NHS in England‚ utilizing laboratory-based‚ quantitative technologies – many employing ELISA.
Private laboratories also offer the test directly to consumers‚ though consulting a doctor for result interpretation is crucial. Accessibility varies geographically; check with your local hospital‚ clinic‚ or online diagnostic services. Ensure the chosen lab uses validated testing methods for accurate and reliable results‚ aiding in appropriate clinical management.

Leave a Reply